By: Cody Gramlich, Physiotherapist
Shoulder pain can be a frustrating issue, as those of you who have experienced it know. You can’t ignore the ache throughout the day, you can’t  reach to grab a plate from the cupboard, or you can’t roll over at night to sleep on your side. This is what one client was struggling with before choosing to start physiotherapy. With a better understanding of his issue and how to manage it, he was able to return to playing pickleball up to five times per week without shoulder pain! One common cause of shoulder pain is commonly referred to as subacromial impingement, or subacromial pain syndrome. In this blog, you will learn what subacromial pain syndrome is, why it is important to understand, and what you can do to manage it.
reach to grab a plate from the cupboard, or you can’t roll over at night to sleep on your side. This is what one client was struggling with before choosing to start physiotherapy. With a better understanding of his issue and how to manage it, he was able to return to playing pickleball up to five times per week without shoulder pain! One common cause of shoulder pain is commonly referred to as subacromial impingement, or subacromial pain syndrome. In this blog, you will learn what subacromial pain syndrome is, why it is important to understand, and what you can do to manage it.
What is Subacromial Pain Syndrome?
You may have previously heard the term or been diagnosed with shoulder impingement. However, there has been movement away from the utilization of this diagnosis in recent years, for two main reasons:
-
- Impingement only describes a compression mechanism of shoulder pain, whereas subacromial pain syndrome is NOT limited to only a compression of structures.
- Shoulder impingement as a diagnosis can be further broken down into four categories on its own.
As a result, subacromial pain syndrome is the most up to date terminology used to describe pain that is located on the lateral aspect (outside) or anterior aspect (front) of your shoulder. This type of shoulder pain is non-traumatic and usually worsened with lifting your arm overhead.
Subacromial pain syndrome is an umbrella term that helps describe pain related to any structures in the subacromial space of the shoulder. Your subacromial space is the region located between the acromion of the scapula (bony prominence on the top of your shoulder) and the head of the humerus. This region is displayed in the image below.
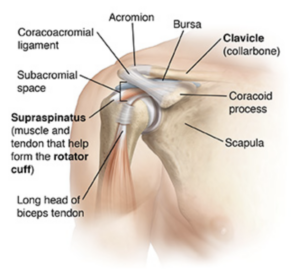
Structures included in the subacromial space5:
-
- Coracoacromial Arch, composed of the Acromion, Coracoid Process and Coracoacromial Ligaments
- Humeral Head
- Subacromial Bursa
- Tendons of the Rotator Cuff; Supraspinatus, Infraspinatus, Teres Minor and Subscapularis
- Tendon of the Long Head of Biceps Brachii
- Coracoacromial ligament
- G-H Joint Capsule
Since so many structures are located in this region, subacromial pain syndrome encompasses a variety of pathologies that may lead to shoulder pain. This includes conditions such as a shoulder bursitis, biceps tendinopathy, or a rotator cuff issue.
Why Is It Important to Understand Subacromial Pain Syndrome?
 Shoulder pain is common and can result in significant loss of function or participation in your day-to-day activities. It is suggested that up to 67% of community dwelling individuals may experience shoulder pain1. 44-65% of all reports of shoulder pain are thought to involve symptoms arising from the subacromial space1. Subacromial pain syndrome is a prevalent issue, so it is important to understand how to prevent and manage it.
Shoulder pain is common and can result in significant loss of function or participation in your day-to-day activities. It is suggested that up to 67% of community dwelling individuals may experience shoulder pain1. 44-65% of all reports of shoulder pain are thought to involve symptoms arising from the subacromial space1. Subacromial pain syndrome is a prevalent issue, so it is important to understand how to prevent and manage it.
Since subacromial pain syndrome is a generic term that encompasses many structures or more specific diagnoses, it is important that you consult a professional to determine which structures may be most affected. Your treatment can be individualized to your specific presentation. This will lead to optimal outcomes, and help you reach your personal goals.
Regardless of the specific pathology or cause of your subacromial pain syndrome, it has been indicated in many studies that physiotherapy can help. One systematic review made a strong recommendation for exercise therapy  as the first-line treatment in subacromial pain syndrome6. A strong recommendation to include manual therapy as an integrated treatment was also made6. Another systematic review even suggested exercise to be as effective as arthroscopic surgery for subacromial pain syndrome3.
as the first-line treatment in subacromial pain syndrome6. A strong recommendation to include manual therapy as an integrated treatment was also made6. Another systematic review even suggested exercise to be as effective as arthroscopic surgery for subacromial pain syndrome3.
Some Risk Factors for Developing Subacromial Pain Syndrome2,5,6
-
- Repetitive movements of the shoulder or hand/wrist during work.
- Work that requires much or prolonged strength of the upper arms.

- Hand-arm vibration (high vibration and/or prolonged exposure) at work.
- Working with a poor ergonomic shoulder posture.
- Altered shoulder kinematics associated with capsular tightness.
- Rotator cuff and scapular muscle dysfunction.
- Age (older).
How Do I Know If I Have Subacromial Pain Syndrome?
-
- No injury or trauma to cause your shoulder pain (gradual onset)
- Pain on the anterior (front) or lateral (outer) aspect of your shoulder.
- Shoulder pain when lifting your arm or with your arm in overhead positions (work or sports with overhead positions).
- Shoulder pain while lying on your affected side.
- Shoulder pain when lifting or holding objects in front of your body.
*Remember that these are the most common symptoms that would indicate you may have subacromial pain syndrome. It may present with different signs/symptoms depending on the individual. If this sounds like you, reach out to a physiotherapist or another healthcare practitioner for a thorough assessment to determine the cause of your specific symptoms.
3 Strategies to Help Manage Your Subacromial Pain Syndrome Symptoms
You may have been struggling with shoulder pain recently and are looking for some guidance. As mentioned earlier, research has consistently shown the benefits of physiotherapy. It even suggests supervised exercise should be the first-line management in subacromial pain syndrome.
1) Postural Awareness
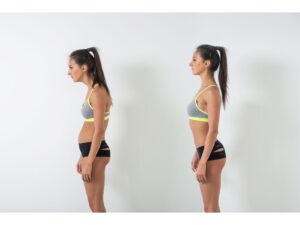
*Being aware of your posture will optimize the position of your shoulders and decrease irritation on structures in the subacromial space. Set a timer for every 30-60 minutes to remind yourself to think about your posture or change up your positioning.
2) Thoracic (Upper Back) Mobility
*Decreased upper back mobility or tension in the muscles of the chest can affect posture or shoulder positioning. The exercise above can help with these areas. Try the exercise with your hands across your chest if it is too uncomfortable to have your hands behind your head. Try 2-3 sets of 8-10 repetitions.
3) Rotator Cuff Strengthening
*Strengthening the rotator cuff muscles allows for better positioning and control of the shoulder with activity. This will help lead to decreased shoulder pain. Try 2-3 sets of 8-12 repetitions.
FAQ
How Long Does It Take Subacromial Pain Syndrome to Heal?
Healing timelines vary for subacromial pain syndrome depending on factors such as your age, activity level, and general health. Some of the strongest positive outcomes for subacromial pain syndrome have been shown with a combination manual therapy and supervised exercise program. It is recommended to see a healthcare professional to determine how you can optimize your healing timelines.
Do I Need Surgery for My Subacromial Pain Syndrome?
Conservative treatment and exercise therapy is the first line of treatment for subacromial pain syndrome. It is suggested that conservative treatment should be considered for up to a year and surgery be contemplated only after exhaustive conservative management5. A healthcare professional will be able to help rule out immediate need for surgery and recommend best treatment options for your subacromial pain syndrome.
What Is the Best Way to Sleep With Subacromial Pain Syndrome?
Typically, sleeping on the affected shoulder will be the most uncomfortable position. The ideal sleeping position will change from individual to individual. Sleeping on your back or sleeping on your unaffected side with the painful shoulder supported by a pillow will likely be the most comfortable positions.
What Comes Next?
Remember, subacromial pain syndrome is non-traumatic pain on the front or outside aspect of your shoulder and is typically worsened with lifting your arm overhead. It is thought to be the most common shoulder issue and can significantly affect your ability to participate in hobbies and work. This is why it is important to be able to identify the signs of subacromial pain syndrome and have a plan to treat and prevent the issue.
Start by trying some of the strategies listed above and see how it goes! Afterwards, it would benefit you to see a physiotherapist in Calgary to guide you through treatment depending on your response.
Feel free to reach out if you have any additional questions on shoulder pain or subacromial pain syndrome or you can book an appointment online by clicking here.
References:
-
- Chaconas E.J., Kolber M.J., Hanney W.J., Daugherty M.L., Wilson S.H., Sheets C. “SHOULDER EXTERNAL ROTATOR ECCENTRIC TRAINING VERSUS GENERAL SHOULDER EXERCISE FOR SUBACROMIAL PAIN SYNDROME: A RANDOMIZED CONTROLLED TRIAL”. International Journal of Sports Physical Therapy. 12 (7): 1121-1133. (2017) doi:10.26603/ijspt20171121
- Diercks, R., Bron, C., Dorrestijn, O., Meskers, C., Naber, R., de Ruiter, T., Willems, J., Winters, J., van der Woude, H. J. (2014). “Guideline for diagnosis and treatment of subacromial pain syndrome”. Acta Orthopaedica, 85 (3), 314–322. (2014) doi:10.3109/17453674.2014.920991
- Haik, M.N., Alburquerque-Sendín, F., Moreira, R.F.C., Pires, E.D., and Camargo, P.R. “Effectiveness of physical therapy treatment of clearly defined subacromial pain: a systematic review of randomised controlled trials”. British Journal of Sports Medicine, 50(18), 1124–1134. (2016) doi:10.1136/bjsports-2015-095771
- Hanratty, C.E., McVeigh, J.G., Kerr, D.P., Basford, J.R., Finch, M.B., Pendleton, A., and Sim, J. “The Effectiveness of Physiotherapy Exercises in Subacromial Impingement Syndrome: A Systematic Review and Meta-Analysis”. Seminars in Arthritis and Rheumatism, 42 (3), 297–316. (2012) doi:10.1016/j.semarthrit.2012.03.015
- Physiopedia 2021. “Subacromial Pain Syndrome”. Physiopedia. Accessed February 15, 2021, https://physio-pedia.com/Subacromial_Pain_Syndrome?utm_source=physiopedia&utm_medium=search&utm_campaign=ongoing_internal
- Pieters, L., Lewis, J., Kuppens, K., Jochems, J., Bruijstens, T., Joossens, L., Struyf, F. “An Update of Systematic Reviews Examining the Effectiveness of Conservative Physical Therapy Interventions for Subacromial Shoulder Pain” Journal of Orthopaedic & Sports Physical Therapy. Volume 50, Issue3, Pages 131-141. (February 2020). https://www.jospt.org/doi/10.2519/jospt.2020.8498
Media References:
Shoulder Anatomy Picture:
-
- Fairview Health Services (2019). “Patient Education: The Shoulder Joint”. Accessed February 26, 2021 via Google Image Search. https://www.fairview.org/patient-education/85899. [Original Source Unknown]
