Written by Vanessa McCrae, Physiotherapist
If you are experiencing pain in your golf swing, if you can’t seem to make that swing correction that you have been working on for months, or if you are just trying to gain a few yards and be more consistent on the golf course – a Golf Movement Assessment might be right for you!
What To Expect
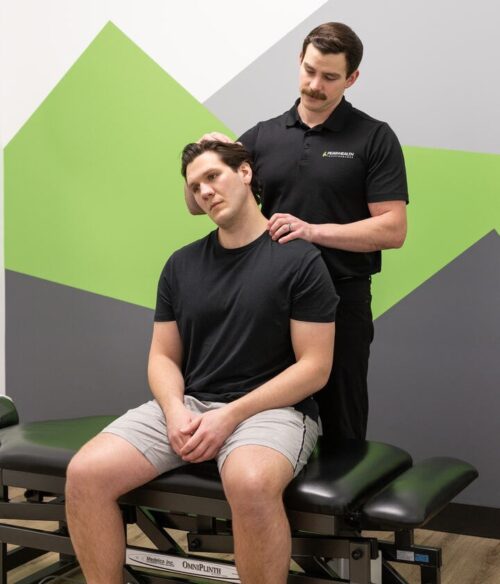
Our Golf Assessment includes a Titleist Performance Institute (TPI) golf-specific movement screen, an orthopaedic assessment, a golf swing video analysis and an individualized exercise program to get you swinging pain-free and efficiently.
What is Titleist Performance Institute?
TPI is the world’s leading educational organization dedicated to the study of how the human body functions in relation to the golf swing. Since its inception in 2003, TPI has studied thousands of golfers ranging from the top professional Tour players to weekend enthusiasts. An incredible amount of data on players of all shapes, sizes, ages, and fitness levels has been gathered during this time.
Using this data, TPI discovered how a properly functioning body allows a player to swing a golf club in the most efficient way possible. Additionally, TPI has analyzed how physical limitations in a player’s body can adversely affect the golf swing and potentially lead to injury.
Who Should Get a Golf Movement Assessment?
Whether you are an avid golfer or someone who is just starting out at the game, a Golf Movement Assessment is for you! An assessment can help you get on the path to adding more yards, having more consistency and playing injury-free! A golf movement assessment is also a great gift to give to anyone in your life who loves the game or seems to complain about aches or pains when playing.
Adding Distance & Improving Consistency
The three main culprits to losing power and consistency in the golf swing are hanging back, losing posture and sliding through impact. While there are many swing drills to help with these issues, more times than not it can be a physical restriction that is preventing you from correcting this problem. Without addressing this restriction, it will be impossible to make the swing change that you have been struggling with.
Injury Prevention 
Estimates suggest that more than 50% of golfers develop chronic problems, the most common being low back pain. The body is designed to have certain joints for mobility and others for stability. A break in this organization can result in undue stress to certain parts of the body.
Due to the high velocity and repetitive nature of the golf swing, the low back tends to be one of the areas that encounter undue stress. Making sure that we have the prerequisite mobility and stability to perform a golf swing will help fend off injuries and allow us to golf all season injury-free!
Unlock Your Best Game Yet!
If you are looking to improve your game this season and play injury-free, then a Golf Movement Assessment is for you! Click here to book today!











 It is important to point out that even after a 2 week intensive, a comprehensive home exercise program can still be created. This is especially true when the child and the therapist providing the therapy intensive have a pre-existing relationship.
It is important to point out that even after a 2 week intensive, a comprehensive home exercise program can still be created. This is especially true when the child and the therapist providing the therapy intensive have a pre-existing relationship.